In this article
Cognitive behavioural therapy, almost always called CBT, is the most researched form of psychotherapy in the world. It has decades of clinical trials supporting its effectiveness for anxiety, depression, OCD, PTSD, phobias, and more. It is also the approach most likely to be recommended by a family doctor or psychiatrist in Ontario when they suggest therapy alongside medication. So what is CBT therapy actually about, and what does it look like in a session?
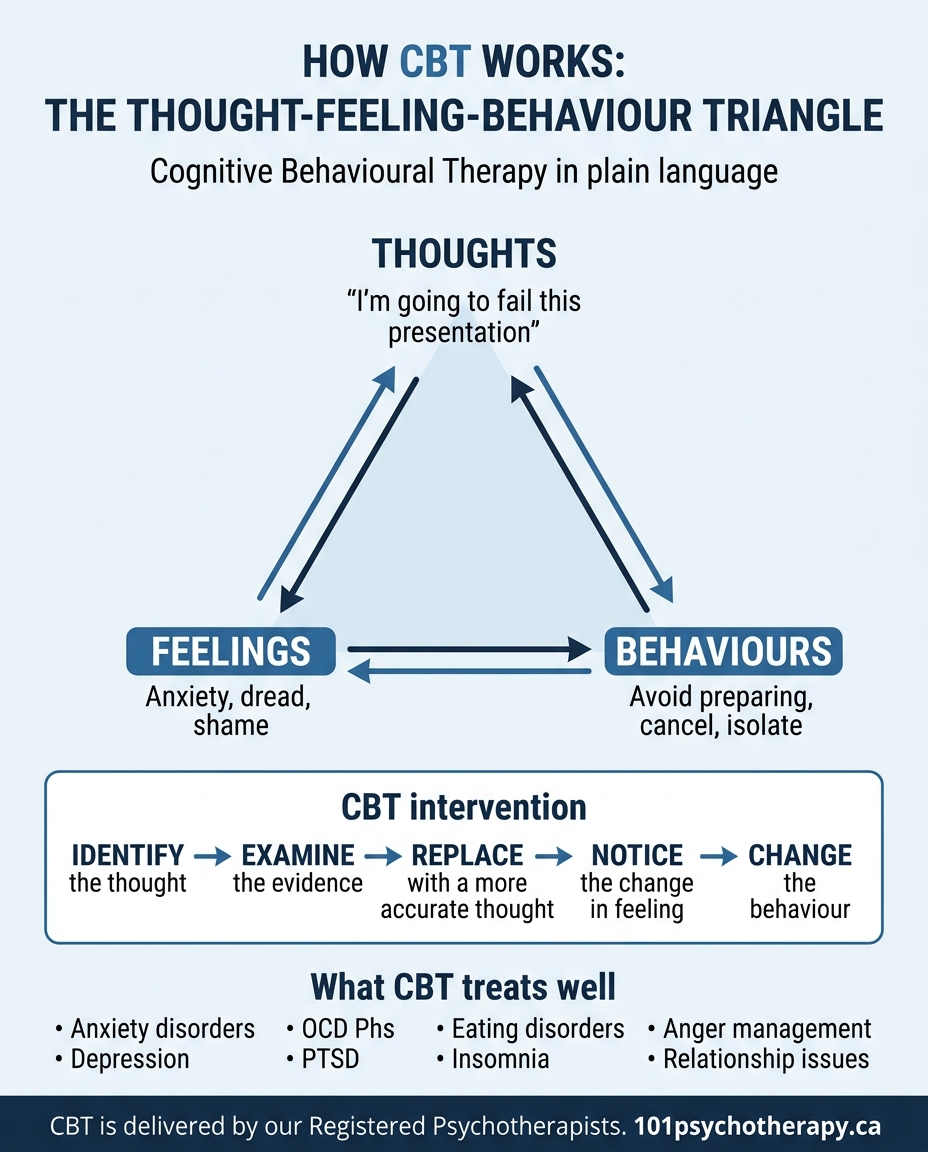
The core idea: thoughts, feelings, and behaviours are connected
CBT is built on one central observation: the way you interpret a situation shapes how you feel about it, which shapes what you do, which shapes how the situation develops, which shapes your next interpretation. A simple example: You send a message to a friend and they do not reply for two days. Interpretation A: They are probably busy. I will follow up later. Feeling: Mild, no real distress. Behaviour: Get on with your day. Interpretation B: They are annoyed with me. I must have said something wrong. Feeling: Anxiety, low-grade dread. Behaviour: Scroll back through your messages looking for what went wrong. Pull back from the friendship. The situation is identical. The interpretation determines everything else. CBT works by targeting the interpretation.

People often ask: Is CBT better than other types of therapy?
CBT has the largest evidence base of any psychotherapy approach, with strong support for anxiety, depression, OCD, PTSD, and health anxiety. That doesn’t make it universally better. Some presentations respond better to EMDR, DBT, ACT, or psychodynamic therapy. A skilled therapist draws from multiple approaches depending on what you’re working on.
Cognitive restructuring: examining and testing your thoughts
The most distinctive CBT technique is cognitive restructuring. In practice, it involves: 1. Identifying automatic thoughts: The quick, often unconscious interpretations that fire in response to a situation. “They did not reply, I must have upset them.” 2. Examining the evidence: What is the evidence for this thought? What is the evidence against it? What are other possible explanations? Is there a more accurate interpretation? 3. Generating a more accurate alternative: Not a positive spin, but a more proportionate and evidence-based version. “They might be busy. I do not know yet. I will find out when I follow up.” This is not about feeling better by thinking better thoughts. It is a more rigorous process of looking at whether your interpretation is actually accurate, and correcting it when it is not.
Did you know?
CBT was developed by Aaron Beck in the 1960s, originally as a treatment for depression. He noticed that his patients’ thinking patterns were as important as their behaviours in maintaining depressed mood. Today, CBT-based treatments are used across more than 50 distinct clinical presentations.
Behavioural techniques: changing what you do
CBT addresses behaviour directly, not just thinking. The two main behavioural approaches are: Behavioural Activation: Particularly useful for depression. When mood is low, people tend to withdraw, reduce activity, and stop doing things that used to bring satisfaction. This reduces sources of positive experience, which worsens the mood. Behavioural activation breaks this cycle by gradually increasing engagement with meaningful or pleasurable activity, even before motivation returns. The insight: motivation follows action more reliably than it precedes it. Exposure: For anxiety, phobias, OCD, and PTSD. Avoidance maintains anxiety because it prevents the nervous system from learning that the feared thing is manageable. Gradual, controlled exposure to feared situations reduces the anxiety response over time through a process called extinction.
What an actual CBT session looks like
CBT sessions are more structured than many people expect. A typical session might include:
- A brief check-in on the week and mood since last session
- Review of homework or between-session practice
- Working on a specific thought pattern, behaviour, or situation
- Learning or practicing a technique (thought record, behavioural experiment, exposure practice)
- Setting homework for the week ahead
The homework component is notable. CBT is not just a weekly conversation. It involves applying what you learn between sessions, which is where much of the change actually happens. This makes it an active, skills-based process rather than a passive one.
How long does a course of CBT take?
For most anxiety and mood conditions, CBT typically runs 12 to 20 sessions, delivered weekly over 3 to 5 months. This is shorter than many other therapy approaches, which is one reason it is often recommended in settings where access, time, or cost is a consideration. Some presentations require longer work, particularly when there are more complex trauma, personality, or relationship factors at play.
Stephanie Sennikov and our other Registered Psychotherapists at 101 Psychotherapy deliver CBT and other evidence-based approaches to clients in Vaughan, Richmond Hill, Aurora, Brampton, and online across Ontario. Book a free consultation to discuss what approach is right for you.
Frequently asked questions
Is CBT the best type of therapy?
CBT has the largest evidence base of any psychotherapy approach for anxiety, depression, OCD, PTSD, and several other conditions. That does not mean it is the best fit for every person or every problem. Some concerns respond better to other approaches, such as EMDR for trauma or ACT for chronic pain and illness. A good therapist will discuss which approach suits your specific situation.
How is CBT different from just thinking positively?
CBT is explicitly not about replacing negative thoughts with positive ones. It is about developing more accurate thoughts. The process involves rigorously examining the evidence for a belief, identifying cognitive distortions, and replacing a distorted thought with a more realistic one, which may still be negative, just proportionate. It is a thinking skill, not a mindset switch.
How long does CBT take to work?
Most people begin noticing meaningful changes within 6 to 8 sessions. Full courses of CBT for anxiety and depression typically run 12 to 20 sessions over 3 to 5 months. This is shorter than many other therapy approaches, which is one reason CBT is favoured in settings where cost or time is a factor.
Can I do CBT on my own without a therapist?
CBT self-help workbooks (like Mind Over Mood) can be genuinely useful for mild to moderate symptoms. Apps like MoodGym and online CBT programs have some research support as well. For moderate to severe symptoms, working with a therapist who can adapt the approach to your specific patterns is more effective. The therapist also catches errors in thinking that you are less likely to spot on your own.
Does CBT work for everyone?
CBT works well for most people, but not equally well for everyone. It requires active participation, willingness to do work between sessions, and a degree of comfort with a more structured, analytical approach. People who prefer more relational, exploratory therapy may find it too structured. It is also less effective when there are unaddressed trauma, personality structure issues, or when the person is not yet ready to engage actively in the process.
Download the free guide
Save this as a free PDF guide.
